Attention Deficit Hyperactivity Disorder (ADHD) and Autism Spectrum Disorder (ASD) are two of the most commonly recognised neurodevelopmental conditions in children and young people [1][2]. Both are typically diagnosed in childhood, and both influence how a person thinks, learns, communicates and regulates behaviour [3].
In the UK, it is estimated that around 700,000 people have a diagnosis of autism [4]. ADHD is also common, with 2,498,000 people in England reportedly having ADHD, including those without a diagnosis [5]. Of these, 741,000 are thought to be children and young people (aged 5-24) [5]. Because ADHD and autism can share certain outward behaviours – such as social difficulties, emotional dysregulation, intense interests or restlessness – parents are often unsure which condition best explains their child’s presentation. In some cases, the answer is not either/or. A child can meet criteria for both [6].
So although ADHD and autism are distinct in their core features, there is meaningful overlap [6]. Here, increasing awareness and updated diagnostic frameworks mean more children are now being recognised and supported than ever before. But understanding where they intersect, and where they differ, remains vitally important in helping families seek appropriate assessment and timely, tailored support.
Where ADHD and Autism Overlap
ADHD and autism both affect how a child processes information, regulates behaviour and responds to the world around them. As a result, certain behaviours may look similar on the surface, particularly in school-aged children [6][7].
Executive functioning differences are common in both. Executive functions are the mental processes responsible for planning, organisation, working memory, time management and impulse control [8][9].
A child may struggle to follow multi-step instructions, forget equipment, leave tasks unfinished or become overwhelmed by larger assignments. These difficulties are often misunderstood as laziness or lack of effort, when in fact they reflect underlying neurodevelopmental differences [10].
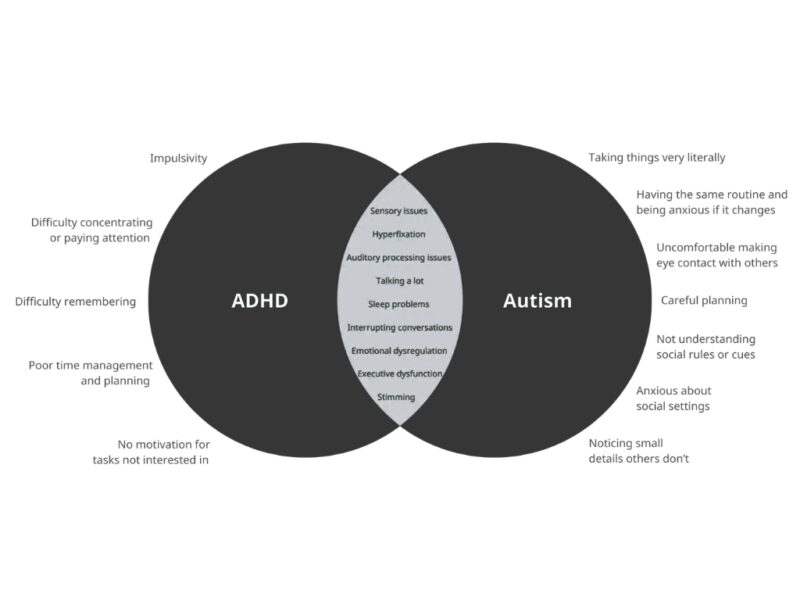
Emotional regulation can also be challenging in both conditions. Children may experience intense frustration, difficulty tolerating disappointment, or rapid escalation of emotions [11][12]. Transitions – such as ending a preferred activity or adapting to unexpected change – can feel disproportionately difficult [13]. Social challenges are another shared feature, although the reasons behind them differ [6][14]. A child with ADHD may interrupt others, dominate conversations or appear not to listen because of impulsivity or distractibility. An autistic child may struggle with reciprocal conversation, interpreting facial expressions or intuitively understanding social rules [15]. In both cases, peer relationships can be affected, sometimes leading to reduced confidence or social withdrawal.
Sensory sensitivities may also occur in both ADHD and autism, though they are more central to autism. Some children may be highly sensitive to noise, clothing textures, bright lights or crowded environments, resulting in overwhelm in busy classrooms or playgrounds. Importantly, dual diagnosis is increasingly recognised [16][17].
Research suggests a significant proportion of autistic children also meet criteria for ADHD. For example, studies have estimated that 50-70% of individuals with autism spectrum disorder also present with ADHD [18].
Key Differences Between ADHD and Autism
Yet despite the overlapping features, ADHD and autism are also defined by different core characteristics.
ADHD mainly affects how a child focuses and controls their impulses. It shows up as ongoing problems with attention and/or high levels of activity and impulsive behaviour that are more extreme than expected for their age and that get in the way of home, school or friendships.19
Inattention may present as difficulty sustaining focus, frequent careless mistakes, forgetfulness in daily activities, losing belongings and difficulty organising tasks. Hyperactivity and impulsivity may include constant fidgeting, difficulty remaining seated, excessive talking, interrupting others, difficulty waiting for a turn and acting without considering consequences.19
In ADHD, attention is often inconsistent. A child may genuinely want to focus but struggle to regulate attention or resist distraction. Social difficulties tend to arise from impulsivity or inattention rather than a fundamental difference in understanding social communication.9
Autism, by contrast, is defined by persistent differences in social communication and interaction, alongside restricted or repetitive patterns of behaviour, interests or sensory experiences.20
Social communication differences in autism may include difficulty interpreting tone of voice or facial expressions, reduced instinctive understanding of social norms, challenges with back-and-forth conversation, or differences in eye contact and non-verbal communication.20
Some autistic children may appear socially withdrawn, while others may be highly verbal but struggle with nuance or flexibility in interaction.210
Restricted or repetitive patterns in autism may manifest as stereotyped or repetitive motor movements, use of objects, or speech (e.g., hand-flapping); insistence on sameness, inflexible adherence to routines, or ritualised patterns (e.g., strong preference for routine or significant distress at unexpected change). It may also result in highly restricted, fixated interests that are abnormal in intensity or focus.20
So while both autism and ADHD can affect learning, relationships and emotional wellbeing, the underlying mechanisms are distinct.
When to Seek Support
Parents often consider professional assessment for ADHD or autism when teachers raise concerns about learning, behaviour or social skills, when home-based strategies no longer suffice, or when challenges persist consistently across multiple settings like school, home and social activities.
These difficulties might include persistent inattention, hyperactivity or impulsivity that interferes with learning or friendships; marked social communication differences such as challenges with back-and-forth conversation, interpreting nonverbal cues or understanding social norms; significant distress linked to routine changes, sensory input or intense interests; or a combination of these patterns that affect daily functioning.
Seeking assessment does not mean labelling your child unnecessarily; it means gaining clarity to replace misunderstandings (like ‘laziness’ or ‘disobedience’) with explanations rooted in neurology, which protects self-esteem and reduces family stress.
Early understanding enables structured, evidence-based supports – such as tailored school plans (e.g., IEPs or 504 Plans), behavioural therapy, medication where appropriate, sensory accommodations, or social skills training – to be implemented sooner, leading to better academic, social and emotional outcomes for both ADHD and autism.21-24
How Assessment Works
For both autism and ADHD, diagnosis is made clinically using established criteria from the DSM-5 or ICD-11 frameworks, through a structured, multi-method assessment process rather than any single test.20,25,26
A comprehensive evaluation includes a detailed developmental history from pregnancy through early milestones, validated questionnaires completed by parents, teachers, and sometimes the child, and direct clinical observation through play-based assessments (e.g. ADOS-2 modules for autism) or cognitive/behavioural tasks revealing attention regulation, social reciprocity, or repetitive patterns.
Symptoms must be present across multiple settings – like home, school, and peers – assessed relative to developmental stage, and causing clear functional impairment to meet diagnostic thresholds.
Where significant overlap is identified – as occurs frequently – a combined assessment protocol is often recommended, screening both conditions simultaneously using tools like the Autism Quotient (AQ) alongside ADHD rating scales.
This approach ensures the full neurodevelopmental picture is understood, preventing missed comorbidities and delivering accurate, proportionate recommendations for supports such as tailored IEPs, therapies, or accommodations.
ADHD and Autism Assessment with The Health Suite Leicester
If you’re unsure whether your child’s challenges align more with ADHD, autism, or both, a comprehensive, consultant-led assessment provides the clarity needed to guide effective support.
At The Health Suite Leicester, we specialise in structured evaluations for ADHD, autism, and co-occurring presentations, following gold-standard clinical frameworks. Our process includes a detailed developmental history, structured parent interviews, validated rating scales from parents and teachers, school observation feedback, and direct clinical observation using tools like ADOS-2 modules where appropriate.
We also routinely screen for common overlapping concerns to ensure recommendations capture your child’s full neurodevelopmental profile and avoid fragmented support.
After assessment, you’ll receive a clear, detailed written report with formal diagnosis (if applicable), practical strategies for home and school, and tailored next steps including behavioural interventions, educational accommodations, therapy options, or medical guidance as needed.
Book your child’s Autism Assessment with expert guidance at The Health Suite.
Visit our related treatment services for Child Autism at The Health Suite Leicester
References:
- Scandurra V, et al. Neurodevelopmental Disorders and Adaptive Functions: A Study of Children With Autism Spectrum Disorders (ASD) and/or Attention Deficit and Hyperactivity Disorder (ADHD). Front Psychiatry. 2019;4;10:673
- Al Ghamdi K, AlMusailhi J. Attention-deficit Hyperactivity Disorder and Autism Spectrum Disorder: Towards Better Diagnosis and Management. Med Arch. 2024;78(2):159-163
- Medical News Today. Is there a link between autism and ADHD in adults? Available at: https://www.medicalnewstoday.com/articles/autism-and-adhd-together-in-adults
- BMA. Autism spectrum disorder. Available at: https://www.bma.org.uk/what-we-do/population-health/improving-the-health-of-specific-groups/autism-spectrum-disorder
- NHS England. ADHD Management Information – May 2025. Available at: https://digital.nhs.uk/data-and-information/publications/statistical/mi-adhd/may-2025
- Martinez S, Stoyanov K, Carcache L. Unraveling the spectrum: overlap, distinctions, and nuances of ADHD and ASD in children. Front Psychiatry. 2024;13;15:1387179
- Wilson AC. Cognitive Profile in Autism and ADHD: A Meta-Analysis of Performance on the WAIS-IV and WISC-V. Arch Clin Neuropsychol. 2024;21;39(4):498-515
- Ceruti C, et al. Comparing Executive Functions in Children and Adolescents with Autism and ADHD-A Systematic Review and Meta-Analysis. Children (Basel). 2024;15;11(4):473
- Townes P, et al. Do ASD and ADHD Have Distinct Executive Function Deficits? A Systematic Review and Meta-Analysis of Direct Comparison Studies. J Atten Disord. 2023;27(14):1571-1582
- Lee RR, et al. Executive Function in Autism: Association with ADHD and ASD Symptoms. J Autism Dev Disord. 2023;53(2):688-700
- Pavlopoulou G, et al. Situating emotion regulation in autism and ADHD through neurodivergent adolescents’ perspectives. Sci Rep. 2025;27;15(1):37464
- Jaisle EM, et al. Linking ADHD and ASD Symptomatology with Social Impairment: The Role of Emotion Dysregulation. Res Child Adolesc Psychopathol. 2023;51(1):3-16
- Restoy D, et al. Emotion regulation and emotion dysregulation in children and adolescents with Autism Spectrum Disorder: A meta-analysis of evaluation and intervention studies. Clinical Psychology Review. 2024; 109: 102410
- Panagiotidi M, Overton PG, Stafford T. Co-Occurrence of ASD and ADHD Traits in an Adult Population. J Atten Disord. 2019;23(12):1407-1415
- Leitner Y. The co-occurrence of autism and attention deficit hyperactivity disorder in children – what do we know? Front Hum Neurosci. 2014;29;8:268
- Autistica. ADHD and autism. Available at: https://www.autistica.org.uk/what-is-autism/adhd-and-autism
- Huang Z, et al. Relationships between Sensory Processing and Executive Functions in Children with Combined ASD and ADHD Compared to Typically Developing and Single Disorder Groups. Brain Sci. 2024;2;14(6):566
- Hours C, Recasens C, Baleyte JM. ASD and ADHD Comorbidity: What Are We Talking About? Front Psychiatry. 2022;28;13:837424
- CDC. Diagnosing ADHD. Available at: https://www.cdc.gov/adhd/diagnosis/index.html
- National Autistic Society. Criteria and tools used in an autism assessment. Available at: https://www.autism.org.uk/advice-and-guidance/diagnosis/assessment-and-diagnosis/criteria-and-tools-used-in-an-autism-assessment
- NHS. Advice about school if your child is autistic. Available at: https://www.nhs.uk/conditions/autism/autism-and-everyday-life/school/
- NICE. Autism spectrum disorder in under 19s: recognition, referral and diagnosis. Available at: https://www.nice.org.uk/guidance/cg128/chapter/recommendations
- NHS. ADHD in children and young people. Available at: https://www.nhs.uk/conditions/adhd-children-teenagers/
- NICE. Attention deficit hyperactivity disorder: diagnosis and management. Available at: https://www.nice.org.uk/guidance/ng87
- Autism Speaks. What are the DSM-5 autism diagnostic criteria? Available at: https://www.autismspeaks.org/autism-diagnostic-criteria-dsm-5
- Gomez R, Chen W, Houghton S. Differences between DSM-5-TR and ICD-11 revisions of attention deficit/hyperactivity disorder: A commentary on implications and opportunities. World J Psychiatry. 2023;19;13(5):138-143
