Osteoarthritis affects millions worldwide, progressively degrading joint cartilage and underlying bone while triggering chronic inflammation that limits daily function.1
In fact, it has never been more timely. The WHO has designated 2021–30 the decade of healthy ageing, highlighting the need to remedy diseases such as osteoarthritis, which strongly affect functional ability and quality of life [1]. The degenerative process associated with osteoarthritis creates a painful cycle where inflamed synovial tissue produces cytokines and prostaglandins that sensitise nerve endings, while swelling and effusion mechanically restrict movement [2].
And the disease can coexist with and negatively affect other chronic conditions, too [1]. Simple activities – walking, climbing stairs, gripping objects, or even sleeping – become increasingly challenging as pain intensifies and supporting muscles weaken from disuse. Inflammation plays a central role beyond structural damage, with the joint capsule thickening, synovial fluid viscosity changing, and osteophytes forming, all contributing to stiffness and reduced range of motion [2][3].
Without intervention, this leads to compensatory movement patterns that stress adjacent joints and accelerate overall physical decline over time.
Understanding Osteoarthritis Pain and Corticosteroid Injection Mechanisms
Treatments targeting osteoarthritic inflammation offer rapid symptom relief, creating opportunities for physiotherapy and exercise programmes that independently reduce disease progression risk by 30-50% when sustained beyond six months [4].
Corticosteroid injections represent one such targeted approach, delivering potent anti-inflammatory medication directly into the joint space to interrupt this inflammatory cascade and restore functional capacity [5][6].
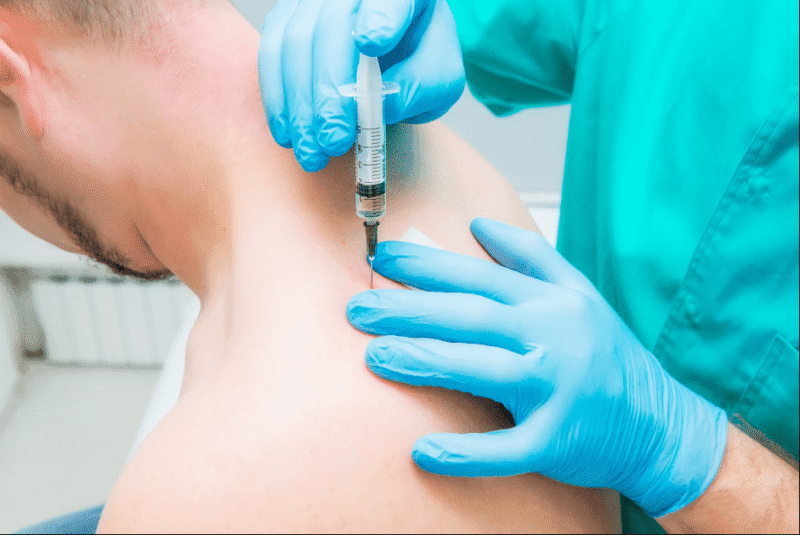
Corticosteroids, also known as glucocorticoids, mimic cortisol – a hormone naturally produced by the adrenal glands to regulate stress and inflammation [7]. When injected intra-articularly, they bind to cytoplasmic receptors in synovial cells and chondrocytes, translocating to the nucleus to suppress inflammatory gene transcription. This multifaceted action inhibits phospholipase A2, reducing arachidonic acid metabolites, including prostaglandins and leukotrienes that drive pain and swelling [8][9].
These medications excel where oral non-steroidal anti-inflammatory drugs (NSAIDs) fail – gastrointestinal intolerance, renal impairment, or cardiovascular contraindications limit systemic therapy for many osteoarthritis patients.
This is because intra-articular (IA) corticosteroids deliver the drug directly to the inflamed joint, achieving higher local bioavailability than systemic administration. This reduces the dose needed and limits side effects like GI or CV risks associated with oral NSAIDs. Studies confirm IA routes provide superior synovial fluid levels with <10% systemic circulation [10].
This targeted delivery means injections are delivered by specialists using evidence-based guidance. Superficial targets include anatomical landmarks – bone prominences, joint lines, muscle bellies. Deeper structures benefit from ultrasound guidance, where precision delivery is considered even more accurate [11][12].
Considering Corticosteroid Injections’ Indications and Suitability
Specifically, corticosteroid injections treat mild-to-moderate osteoarthritis across weight-bearing and upper limb joints, plus related tendinopathies including lateral epicondylitis (tennis elbow), plantar fasciitis, patellar tendinopathy, shoulder/hip/knee tendinopathy, and Achilles tendinopathy [13] [14].
Optimal candidates exhibit persistent pain despite optimised oral/topical therapy, joint effusion limiting physiotherapy progress, symptom flares blocking sleep, work, or caregiving, or NSAID contraindications such as GI bleed history, renal impairment, or heart failure [15][16].
NICE guidelines (UK’s gold-standard recommendations) endorse intra-articular corticosteroid injections precisely for these scenarios – when oral treatments fail, prove unsuitable, or cause side effects [16]. This is because they offer reliable pain relief across the knee, hip, hand and other joints, empowering individuals to re-engage with essential physiotherapy and restore function.
In this way, injections prove strategic within stepped-care pathways: first-line paracetamol/exercise, second-line topical NSAIDs/physiotherapy, third-line injections bridging to viscosupplementation, bracing, or surgical evaluation.
Examining the Clinical Evidence and Outcomes For Corticosteroid Injections
Studies and systematic reviews provide robust evidence for corticosteroid injections in osteoarthritis management. For example, a landmark analysis of 27 randomised controlled trials involving 2,267 patients demonstrated that intra-articular knee injections reduced pain by 2.0 points on a 10-point visual analogue scale at one month compared to placebo, with a number-needed-to-treat of just 5 for clinically meaningful improvement [17].
This efficacy extends across multiple joints. Shoulder injections improve range of motion by 25-35 degrees within two weeks, while hip injections reduce WOMAC pain scores by 28% at three months. Pain reduction manifests rapidly; 50-70% improvement emerges within 72 hours, peaking at 70-85% by week two. Functional gains follow closely; timed up-and-go tests improve by 2.5 seconds and 6-minute walk distances increase by 35 metres [9].
Trials combining injections with structured exercise demonstrate 40% greater functional gains versus exercise alone, as reduced pain enables higher training intensity and better compliance. Sleep disturbance resolves among 75% within one week, enhancing work capacity and caregiving ability [9][17].
This efficacy comes at the same time as proven safety. Controlled trials show no accelerated cartilage damage, with complication rates under 1% when using ultrasound guidance (>95% accuracy vs 70-85% blind). At the same time, systemic effects remain minimal compared to oral steroids, making injections ideal for NSAID-intolerant patients [18].
Choosing The Health Suite for Osteoarthritis Relief
Deciding whether corticosteroid injections suit your osteoarthritis requires a thorough clinical assessment. Persistent pain patterns despite optimised therapy, joint effusion limiting physiotherapy, NSAID contraindications, or flares disrupting sleep and work all guide appropriate candidacy within established stepped-care pathways. For suitable patients, these targeted injections create essential windows of pain relief and restored mobility, enabling active participation in rehabilitation programmes that independently slow osteoarthritis progression. When combined with specialist physiotherapy, this approach transforms short-term symptom control into sustained functional gains and improved quality of life.
At The Health Suite, corticosteroid injections form a cornerstone of comprehensive rheumatology services, delivered through a personalised, patient-centred framework. Skilled specialists integrate advanced diagnostic assessment – including musculoskeletal ultrasound – with tailored treatment planning that considers complete medical history, biomechanics, and lifestyle factors influencing joint health.
The Health Suite offers both non-guided injections for superficial targets and ultrasound-guided precision (>95% accuracy), ensuring optimal medication delivery while minimising risks. Treatment seamlessly coordinates with physio-led consultations, structured rehabilitation, and long-term strategies to maintain joint function and prevent decline. The Health Suite Leicester provides expert medical guidance from experienced rheumatology, physiotherapy and osteopathy specialists, personalised treatment plans matching specific conditions and goals, and compassionate care ensuring comfort and confidence throughout the entire process.
Relieve osteoarthritis pain and restore mobility with specialist corticosteroid injections.
Visit our related treatment services for Osteoarthritis
References:
- GBD 2021 Osteoarthritis Collaborators. Global, regional, and national burden of osteoarthritis, 1990-2020 and projections to 2050: a systematic analysis for the Global Burden of Disease Study 2021. Lancet Rheumatol. 2023; 21;5(9):e508-e522
- Yunus MHM, Nordin A, Kamal H. Pathophysiological Perspective of Osteoarthritis. Medicina (Kaunas). 2020; 16;56(11):614
- Scanzello CR, Goldring SR. The role of synovitis in osteoarthritis pathogenesis. Bone. 2012;51(2):249-57
- Lawford BJ, et al. Exercise for osteoarthritis of the knee. Cochrane Database of Systematic Reviews. 2024;12: CD004376
- Jüni P, et al. Intra‐articular corticosteroid for knee osteoarthritis. Cochrane Database of Systematic Reviews. 2015;10: CD005328
- Singer B, et al. Corticosteroid Use in Musculoskeletal and Neuraxial Interventions: Effects on Glycemic Control. Medicina (Kaunas). 2025; 21;61(5):936
- Ramamoorthy S, Cidlowski JA. Corticosteroids: Mechanisms of Action in Health and Disease. Rheum Dis Clin North Am. 2016;42(1):15-31, vii
- Ayhan E, Kesmezacar H, Akgun I. Intraarticular injections (corticosteroid, hyaluronic acid, platelet rich plasma) for the knee osteoarthritis. World J Orthop. 2014; 18;5(3):351-61
- Choueiri M, Chevalier X, Eymard F. Intraarticular Corticosteroids for Hip Osteoarthritis: A Review. Cartilage. 2021;13(1_suppl):122S-131S
- Jones IA, et al. Intra-articular treatment options for knee osteoarthritis. Nat Rev Rheumatol. 2019;15(2):77-90
- Kumar Sahu A, Rath P, Aggarwal B. Ultrasound-guided injections in musculo-skeletal system – An overview. J Clin Orthop Trauma. 2019;10(4):669-673
- Benzon HT, et al. Use and safety of corticosteroid injections in joints and musculoskeletal soft tissue: guidelines from the American Society of Regional Anesthesia and Pain Medicine, the American Academy of Pain Medicine, the American Society of Interventional Pain Physicians, and the International Pain and Spine Intervention Society. Reg Anesth Pain Med. 2025; 12:rapm-2024-105656
- Wehling P, et al. Effectiveness of intra-articular therapies in osteoarthritis: a literature review. Therapeutic Advances in Musculoskeletal Disease. 2017;9(8):183-196
- Jones IA, et al. Intra-articular treatment options for knee osteoarthritis. Nat Rev Rheumatol. 2019;15(2):77-90
- Hodgens A, Sharman T. Corticosteroids. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. 2025. Available at: https://www.ncbi.nlm.nih.gov/books/NBK554612/
- NICE. Osteoarthritis in over 16s: diagnosis and management. Available at: https://www.nice.org.uk/guidance/ng226
- Arroll B, Goodyear-Smith F. Corticosteroid injections for osteoarthritis of the knee: meta-analysis. BMJ. 2004; 10;328(7444):869
- AAOS. Management of Osteoarthritis of theKnee (Non-Arthroplasty). Available at: https://www.aaos.org/globalassets/quality-and-practice-resources/osteoarthritis-of-the-knee/oak3cpg.pdf
