Hyaluronic acid is a naturally occurring substance found throughout the human body, with particularly high concentrations in connective tissue, skin, eyes, and synovial fluid within joints [1].
Its primary biological role is to retain water, maintain tissue hydration, and support lubrication and shock absorption in areas exposed to repeated mechanical stress [2][3].
Within joints, hyaluronic acid contributes to smooth, low-friction movement, supporting everyday activities such as walking, bending, and climbing stairs. It also helps protect cartilage surfaces by distributing load and reducing mechanical strain.
Over time, however, natural hyaluronic acid levels decline as part of the ageing process and in response to cumulative physical stress, inflammation, and injury. As a result, injectable hyaluronic acid has become an increasingly used therapeutic option within musculoskeletal care, going beyond the shortcomings of injectable steroids [4].
Hyaluronic acid injections aim to support joint comfort and movement by restoring some of the viscoelastic properties of synovial fluid, thereby improving the internal joint environment. They are widely explored by individuals seeking non-surgical, joint-supportive interventions that help maintain activity and mobility [5].
Understanding how effective hyaluronic acid injections are – and how best to support optimal outcomes – requires an appreciation of both their biological role and the clinical evidence underpinning their use.
Understanding Hyaluronic Acid and Joint Function
Hyaluronic acid is composed of repeating molecular units that allow it to bind large volumes of water relative to its size. This unique structure is why it helps to maintain hydration, elasticity, and shock absorption within tissues [4].
In synovial joints, hyaluronic acid plays a central role in determining the quality of synovial fluid. During slow movements, it acts primarily as a lubricant, reducing friction between joint surfaces. And during faster or higher-impact activity, it behaves more elastically, helping to absorb mechanical forces. This dual function is essential for joint efficiency, comfort, and resilience [6].
When hyaluronic acid levels decline or its molecular structure becomes altered, synovial fluid loses some of its protective capacity. This can increase friction, elevate mechanical stress on cartilage, and heighten sensitivity within the joint. Over time, these changes may manifest as stiffness, discomfort, and reduced range of motion [6][7].
In addition to its mechanical effects, research suggests that hyaluronic acid may also influence local signalling pathways involved in inflammation and pain modulation, further supporting its therapeutic role [6][8].
Looking at the Clinical Evidence for Effectiveness
Hyaluronic acid injections have been widely studied within musculoskeletal medicine, with a substantial body of clinical research examining their impact on joint comfort, stiffness, and functional movement.
Unlike injectable steroids, improvements tend to develop gradually rather than immediately, often becoming more noticeable several weeks after administration. This delayed onset reflects the time required for synovial fluid properties and joint biomechanics to adapt. In many cases, benefits are sustained for several months, supporting ongoing movement and activity [9].
Importantly, although clinical responses vary, a meaningful proportion of patients achieve symptom improvements that exceed commonly accepted thresholds for clinical relevance, with meta-analyses showing statistically significant benefits in both pain and function versus placebo. In practice, these changes are frequently reflected in better walking tolerance, reduced activity-related discomfort, and improvements in patient-reported quality-of-life measures [9].
For example, in clinical studies of knee osteoarthritis, people receiving hyaluronic acid injections often report average pain reductions in the region of 10-20 points on a 0-100 scale, with improvements generally becoming most noticeable between 4 and 8 weeks after treatment [9].
Rather than being just a quick fix, hyaluronic acid injections are better thought of as a joint-supportive treatment that helps your joints move more smoothly and comfortably over time. Instead of chasing instant relief, the goal is to gradually improve how the joint feels and functions so you can stay active for longer.
Recognising the Role of Hyaluronic Acid in Osteoarthritis Care
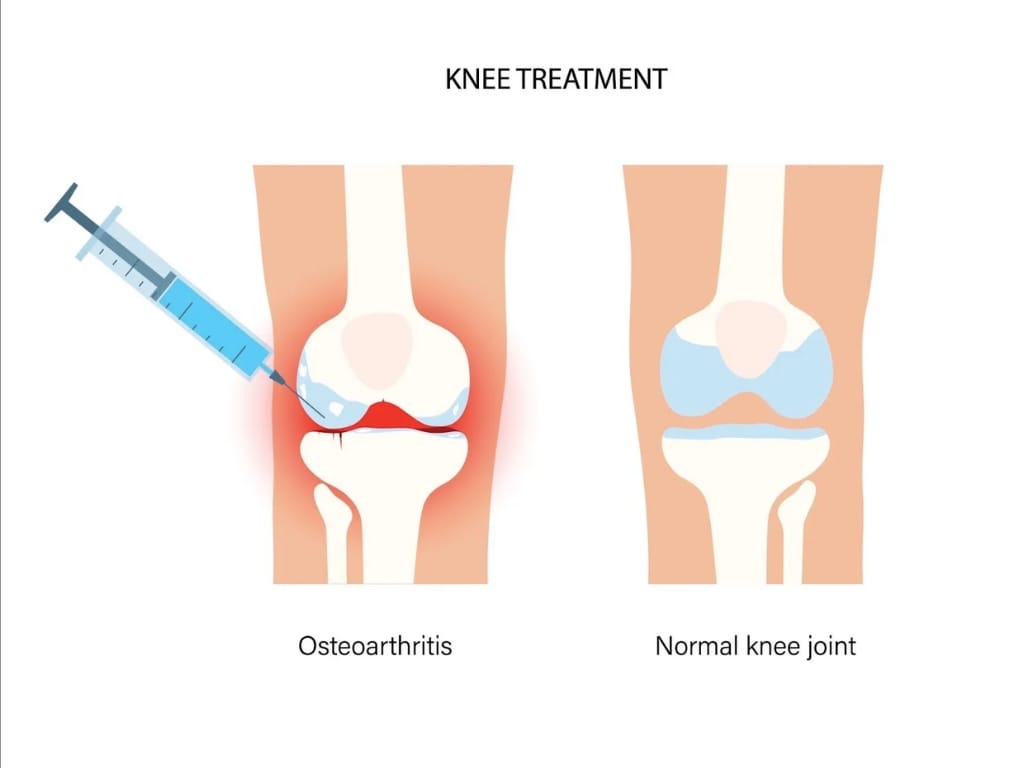
One of the most established uses of hyaluronic acid injections is in the management of osteoarthritis, a chronic degenerative joint disease involving inflammation and structural changes, most commonly affecting weight‑bearing joints such as the knee [10].
Osteoarthritis affects over 10 million people in the UK – roughly one in five adults – and is a leading cause of disability, particularly among those over 50 [11]. This makes it one of the most common chronic conditions managed in UK primary care, with knee osteoarthritis alone accounting for a significant share of GP visits and joint replacement referrals [11][12].
The disease is characterised by joint pain, stiffness, and progressive loss of function that develops gradually over many years, often starting subtly before impacting daily activities like walking or climbing stairs [11][12].
This is because within osteoarthritic joints, both the concentration and molecular quality of endogenous hyaluronic acid are reduced. Synovial fluid becomes less viscous and less effective at lubrication and shock absorption, contributing to increased mechanical strain and symptom burden [6].
Clinical evidence suggests that hyaluronic acid injections may be particularly helpful in individuals with mild to moderate osteoarthritis, where joint structure is still relatively preserved. In these cases, improving synovial fluid properties can support movement, reduce discomfort, and help maintain activity levels [4].
For example, a 2025 systematic review of randomised trials found hyaluronic acid injections led to significant long-term improvements in pain and function, specifically in early-stage osteoarthritis patients (Kellgren-Lawrence grades 1-2), particularly older women, despite initial symptom worsening [13].
That’s why, for many individuals, hyaluronic acid injections form part of a conservative management approach, supporting symptom relief while aiming to preserve joint function and delay more invasive interventions.
Considering Who is Most Likely to Benefit
Response to hyaluronic acid injections is influenced by several interrelated factors.
- Disease stage is among the most important, with earlier intervention generally associated with more favourable outcomes. Individuals with preserved joint space and lower levels of structural change (such as Kellgren-Lawrence grades 1-2) tend to experience greater improvements in comfort and mobility [14].
- Functional goals and activity levels also shape perceived effectiveness. People seeking to remain active, return to low-impact exercise, or improve day-to-day movement often report greater benefit, particularly when injections allow more comfortable participation in rehabilitation or physical activity [15].
- Metabolic health may further influence response. Excess body weight increases mechanical load on joints, while systemic low-grade inflammation can affect tissue resilience. Addressing these factors alongside injections may help optimise and sustain outcomes [16].
In addition, hyaluronic acid formulations vary in molecular weight, structure, and dosing schedules. Evidence suggests that careful product selection and precise injection technique play an important role in achieving consistent and meaningful results [17].
Taken together, these considerations reinforce the importance of an individualised, clinician-led approach.
Supporting Results Through an Integrated Strategy
Hyaluronic acid injections are most effective when used as part of a broader joint-health strategy rather than as a standalone solution. Contemporary understanding of joint conditions recognises the importance of the combined influence of biomechanics, muscle strength, metabolic health, and lifestyle factors alongside structural change [14][17].
Within this, exercise therapy remains central. Strengthening the muscles surrounding affected joints reduces mechanical load, improves stability, and enhances movement efficiency. When injections improve joint comfort, individuals are often better able to engage fully in physiotherapy and regular physical activity, amplifying overall benefit [18].
Weight management is also key. Even modest reductions in body weight can significantly decrease joint loading, particularly at the knee. Nutritional approaches that support metabolic health and reduce inflammatory burden may further enhance joint resilience and responsiveness to treatment [15].
Adequate hydration, protein intake, and micronutrients involved in connective tissue support also play a role in tissue repair and adaptation. While lifestyle measures cannot reverse structural joint changes, they help create an internal environment in which therapeutic interventions can work more effectively [16][19].
Applying a personalised, clinic-led approach with The Health Suite
Deciding whether hyaluronic acid injections are appropriate involves careful clinical assessment. Symptom pattern, movement limitations, imaging findings, activity goals, and previous treatment responses all inform this process. For many individuals, injections provide a valuable window of improved comfort and mobility, enabling greater participation in rehabilitation and lifestyle change. When aligned with tailored exercise, nutritional guidance, and ongoing support, this can contribute to more sustainable joint health outcomes.
At The Health Suite Leicester, hyaluronic acid injections are considered within a personalised, integrative framework of care. Assessment extends beyond the joint itself to consider biomechanics, metabolic health, inflammation, and lifestyle influences that shape symptom experience and recovery. Where appropriate, injections may be integrated with targeted rehabilitation, nutritional support, and long-term strategies aimed at maintaining movement, function, and quality of life.
Explore how The Health Suite’s personalised approach could relieve your joint pain and support long-term movement.
References:
- Papakonstantinou E, Roth M, Karakiulakis G. Hyaluronic acid: A key molecule in skin aging. Dermatoendocrinol. 2012; 1;4(3):253-8.
- Pereira TV, et al. Viscosupplementation for knee osteoarthritis: systematic review and meta-analysis. BMJ. 2022; 6;378:e069722
- Xing D, et al. Intra-articular Hyaluronic Acid in Treating Knee Osteoarthritis: a PRISMA-Compliant Systematic Review of Overlapping Meta-analysis. Sci Rep. 2016; 12;6:32790
- Trigkilidas D, Anand A. The effectiveness of hyaluronic acid intra-articular injections in managing osteoarthritic knee pain. Ann R Coll Surg Engl. 2013;95(8):545-51
- Altman RD, et al. The mechanism of action for hyaluronic acid treatment in the osteoarthritic knee: a systematic review. BMC Musculoskelet Disord. 2015; 26;16:321
- Tamer TM. Hyaluronan and synovial joint: function, distribution and healing. Interdiscip Toxicol. 2013;6(3):111-25
- Karatay S, K, et al. Effects of different hyaluronic acid products on synovial fluid NO levels in knee osteoarthritis. Clin Rheumatol. 2005;24(5):497-501
- Chrostek L, Cylwik B. Hyaluronic Acid in Immune Response. Biomolecules. 2025; 14;15(7):1008
- Trigkilidas D, Anand A. The effectiveness of hyaluronic acid intra-articular injections in managing osteoarthritic knee pain. Ann R Coll Surg Engl. 2013;95(8):545-51
- Chavda S, Rabbani SA, Wadhwa T. Role and Effectiveness of Intra-articular Injection of Hyaluronic Acid in the Treatment of Knee Osteoarthritis: A Systematic Review. Cureus. 2022; 26;14(4):e24503
- Arthritis UK. The State of Musculoskeletal Health 2025. Arthritis and other musculoskeletal conditions in numbers. Available at: https://www.arthritis-uk.org/media/flpbvm2m/arthritisuk_state_of_msk_health_-report_2025.pdf
- Swain S, et al. Trends in incidence and prevalence of osteoarthritis in the United Kingdom: findings from the Clinical Practice Research Datalink (CPRD). Osteoarthritis and Cartilage. 2020; 28:6:792-801
- Migliorini F, et al. Intra-articular Hyaluronic Acid Injections May Be Beneficial in Patients with Less Advanced Knee Osteoarthritis: A Systematic Review of Randomised Controlled Trials. Sports Med. 2025;55(8):1953-1969
- Chen Y, et al. Quantitative analysis of the efficacy and associated factors of intra-articular hyaluronic acid…A systematic review of randomized trials. Osteoarthritis and Cartilage. 2025; 33(6):666-679
- Glinkowski WM, Tomaszewski W. Intra-Articular Hyaluronic Acid for Knee Osteoarthritis: A Systematic Umbrella Review. J Clin Med. 2025; 14;14(4):1272
- Migliore A, Procopio S. Effectiveness and utility of hyaluronic acid in osteoarthritis. Clin Cases Miner Bone Metab. 2015;12(1):31-3
- Ferkel E, et al. Intra-articular Hyaluronic Acid Treatments for Knee Osteoarthritis: A Systematic Review of Product Properties. Cartilage. 2023;14(4):424-432
- Sherman SL, et al. Mechanisms of Action of Intra-articular Hyaluronic Acid Injections for Knee Osteoarthritis: A Targeted Review of the Literature. The American Journal of Sports Medicine. 2025;53(11):2771-2782
- Liao CD, et al. Effects of Protein-Rich Nutritional Composition Supplementation on Sarcopenia Indices and Physical Activity during Resistance Exercise Training in Older Women with Knee Osteoarthritis. Nutrients. 2021; 21;13(8):2487