Most people are broadly familiar with the cardiovascular system, the heart, arteries and veins that keep blood circulating around the body. Far fewer give much thought to the lymphatic system, the equally essential but considerably less celebrated network that runs alongside it. Yet the lymphatic system is fundamental to immunity, fluid balance and the body’s ability to clear waste, and when it is not functioning well, the effects are felt across the whole body [1].
Lymphatic drainage therapy is a specialist treatment designed to support and stimulate the lymphatic system, helping it to do what it is naturally meant to do more effectively: keep the body’s internal environment clean, balanced and defended. Interest in the therapy has grown considerably in recent years, both within clinical medicine, where it has a well-established evidence base in specific conditions, and among people seeking to support their general health and recovery [2][3].
Understanding what the lymphatic system actually does, what happens when it becomes compromised, and what lymphatic drainage therapy involves is the foundation for making any informed decision.
What the Lymphatic System Does
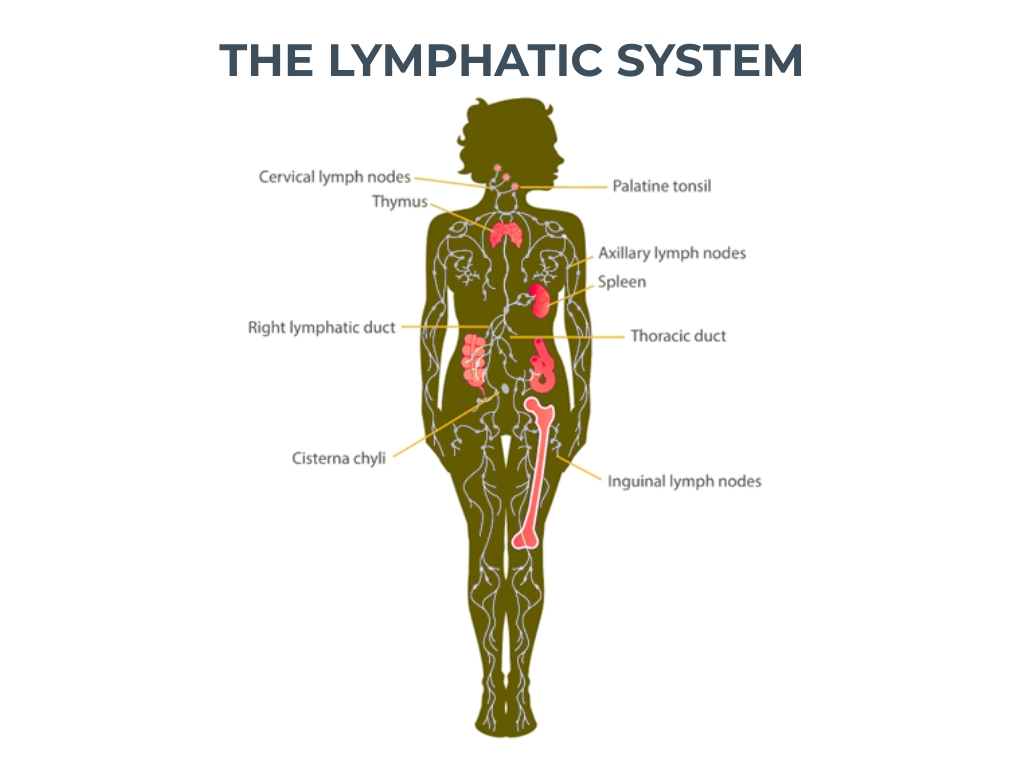
The lymphatic system is a network of vessels, lymph nodes, organs and tissues that runs throughout the body and serves three primary functions:
- Maintaining fluid balance: it helps return excess fluid, proteins and waste products from the tissues back into the bloodstream
- Supporting immune function:
- It acts as a filtering and surveillance system, allowing the body to detect and respond to infection, abnormal cells and foreign material
- It transports immune cells around the body, helping coordinate immune defence
- And absorbing dietary fats from the digestive system – in the gut, specialised lymphatic vessels called lacteals help absorb fat-soluble nutrients, not just fats alone.
As blood circulates through the capillaries, a portion of the plasma it carries leaks out into the surrounding tissues, bathing cells in fluid that delivers nutrients and collects waste products.
Most of this fluid is reabsorbed directly back into the capillaries, but around 10-15% of it is not, and without a mechanism for returning it to circulation, it would accumulate in the tissues, causing swelling and disrupting normal cellular function [4]. The lymphatic system provides that mechanism. Lymphatic capillaries absorb this excess interstitial fluid, now called lymph, and transport it through a network of progressively larger vessels, through lymph nodes where it is filtered and patrolled by immune cells, and ultimately back into the bloodstream via the thoracic duct [1][5].
The immune function of the lymphatic system is equally important. Lymph nodes are densely populated with lymphocytes and macrophages, the white blood cells responsible for identifying and destroying pathogens, abnormal cells and foreign material. When infection or inflammation is present, lymph nodes become active, sometimes noticeably swollen, as the immune response is mounted [5][6]. The spleen, thymus and tonsils are all components of the broader lymphatic system and play important roles in immune surveillance and response.
Unlike the cardiovascular system, the lymphatic system has no dedicated pump. Lymph moves through the vessels primarily as a result of the contractions of surrounding skeletal muscle, respiratory movements, arterial pulsation and the gentle intrinsic contractions of the lymphatic vessel walls themselves [7]. This means that the lymphatic system is inherently dependent on breathing and physical activity to function optimally, and that when these are reduced, lymphatic flow can slow significantly.
When the Lymphatic System Struggles
The lymphatic system is resilient, but it can become compromised in ways that produce recognisable symptoms and have meaningful consequences for wellbeing. Lymphoedema is the most clinically significant lymphatic condition, occurring when the lymphatic system is unable to drain fluid adequately from a region of the body, resulting in chronic swelling, heaviness, skin changes and increased risk of infection in the affected area. It affects an estimated 200,000 people in the UK [3][8].
Persistent puffiness or fluid retention, particularly in the face, hands, ankles or abdomen, unexplained fatigue, a sense of heaviness in the limbs, recurrent infections or a feeling of general sluggishness that does not resolve with rest are all symptoms that may reflect reduced lymphatic efficiency [3][7]. These experiences, while not always meeting the threshold for a clinical diagnosis, can significantly affect daily comfort and quality of life. Now, with the increasingly sedentary nature of modern life, combined with high levels of chronic stress, suboptimal lymphatic function is more prevalent than is commonly appreciated.
What Lymphatic Drainage Therapy Involves
Manual lymphatic drainage (MLD) is a specialist therapeutic technique refined and validated through decades of clinical research and practice [9]. It involves the application of precise, rhythmic, light-pressure movements to the skin in the direction of lymphatic flow, using specific sequences and techniques designed to stimulate the gentle contractions of lymphatic vessel walls and encourage the movement of lymph through the system.
The pressure used in MLD is considerably lighter than that used in conventional massage, reflecting the superficial location of the lymphatic capillaries in the skin and the gentle nature of the pumping mechanism being stimulated. Heavy pressure compresses the lymphatic vessels rather than encouraging them to contract, which is why standard deep tissue massage does not produce the same lymphatic effects and why MLD requires specific training to perform correctly [9][10].
A typical MLD session begins with work at the lymph node clusters in the neck, axilla and groin, which are cleared first to create capacity for the lymph moving towards them from the periphery. The therapist then works systematically through the affected regions, using light, rhythmic strokes that follow the anatomical pathways of the lymphatic vessels [11]. Sessions typically last between 45 and 90 minutes, depending on the area being treated and the clinical indication.
What the Evidence Shows
From post-surgical recovery to chronic disease management, MLD has grown substantially over recent decades. And importantly, its benefits are not limited to those with a diagnosed medical condition. Many people without any clinical diagnosis report meaningful improvements in energy, reduced puffiness and a general sense of feeling lighter and better after a course of treatment, and there is a growing body of research examining these broader wellbeing effects.
In the management of lymphoedema, the evidence base is particularly well established. A Cochrane review examining MLD in the treatment of breast cancer-related lymphoedema found that MLD combined with compression bandaging produced significantly greater reductions in limb volume than compression bandaging alone, and that MLD was well tolerated with no serious adverse effects reported across the studies reviewed [11].
The review supported the inclusion of MLD as a core component of combined decongestive therapy, a finding that has since been reflected in national and international lymphoedema management guidelines [12]. The post-surgical application of MLD is also well supported, with studies showing MLD performed in the weeks following surgery significantly reduced post-operative bruising and recovery time compared with standard post-operative care [13].
Evidence also supports the use of lymphatic drainage in the management of fibromyalgia and chronic musculoskeletal pain. A randomised controlled trial published in the Journal of Back and Musculoskeletal Rehabilitation found that patients with fibromyalgia who received MLD reported significantly greater reductions in pain intensity, fatigue and morning stiffness compared with those receiving connective tissue massage, with improvements in sleep quality also noted [14]. And for those seeking lymphatic drainage purely for general health and wellbeing, the rationale is grounded in the same physiology. When lymphatic flow is optimised, the body becomes more efficient at clearing metabolic waste, regulating fluid and maintaining immune surveillance [1][7].
Research examining the physiological effects of MLD in healthy individuals has found that even a single session produces measurable increases in lymphatic flow velocity and reductions in tissue fluid accumulation, providing a biological basis for the improvements in energy, reduced bloating and general sense of vitality that many people report following treatment [15].
In fact, a broader systematic review examining the therapeutic applications of MLD across multiple conditions found consistent evidence of benefit in reducing oedema, improving tissue perfusion and reducing pain and fatigue across a wide range of presentations, concluding that MLD represents a safe, well-tolerated intervention with applications extending well beyond its original use in lymphoedema management [16].
Who Can Benefit from Lymphatic Drainage Therapy
Lymphatic drainage therapy has a wide range of applications, and it is worth saying clearly that you do not need a diagnosis to benefit from lymphatic drainage therapy. Many people come to MLD simply because they want to feel better, whether that means less puffiness in the morning, more energy through the day, faster recovery after exercise or illness, or a general sense of their body functioning more smoothly.
Used in this way, MLD is a supportive, preventative therapy that works with the body’s natural systems rather than treating a specific condition, and it is entirely appropriate for people who are otherwise well. For those with a clinical need, the evidence base is particularly strong. People with diagnosed lymphoedema, whether primary or secondary, represent the group with the clearest and most well-evidenced indication for MLD as part of a comprehensive management programme [8][13].
People recovering from surgery, whether major reconstructive procedures or cosmetic interventions, frequently benefit from post-operative MLD to reduce swelling, accelerate tissue healing and improve comfort during recovery [15]. It may also benefit with chronic fatigue, recurrent infections or a persistent sense of physical sluggishness that has not responded to other interventions. They may find that lymphatic drainage therapy provides meaningful improvement in energy levels and general wellbeing [3][7].
Manual Lymphatic Drainage Therapy at The Health Suite Leicester
Whether you are managing a diagnosed lymphatic condition, recovering from surgery or treatment, or simply looking to support your body’s natural systems and improve how you feel day to day, lymphatic drainage therapy offers a gentle, evidence-based intervention with a broad range of potential benefits.
At The Health Suite Leicester, our lymphatic drainage therapy is delivered by specialist practitioners with the clinical training and expertise to tailor treatment to your individual needs.
We begin with a thorough assessment to understand your health history, identify the most appropriate treatment approach, and ensure that lymphatic drainage therapy is safe and well-suited to your circumstances. Treatment is delivered in a calm, supportive environment with clear guidance on what to expect and how to support the benefits of therapy between sessions.
Book your lymphatic drainage session today!
Book supportive treatments for lymphatic drainage
Read our clinically validated blog on the supportive treatments for lymphatic drainage
References:
- Swartz MA. The physiology of the lymphatic system. Adv Drug Deliv Rev. 2001;50(1–2):3–20
- Williams A. Manual lymphatic drainage: exploring the history and evidence base. Br J Community Nurs. 2010;15(4):S18–S24
- International Lymphoedema Framework. Best Practice for the Management of Lymphoedema. London: MEP; 2006. Available at: https://www.lympho.org/uploads/files/files/Best_practice.pdf
- Guyton AC, Hall JE. Textbook of Medical Physiology. 13th ed. Philadelphia: Elsevier; 2016
- Rockson SG. Lymphatics: where the circulation meets the immune system. Lymphat Res Biol. 2013;11(3):115–116
- Alitalo K. The lymphatic vasculature in disease. Nat Med. 2011;17(11):1371–1380
- Földi M, Strössenreuther R. Foundations of Manual Lymph Drainage. 3rd ed. Edinburgh: Elsevier Mosby; 2005
- Lymphoedema Support Network. What Is Lymphoedema? Accessed 2025. Available at: https://www.lymphoedema.org/information/what-is-lymphoedema/
- Williams A. Manual lymphatic drainage: exploring the history and evidence base. Br J Community Nurs. 2010;15(4):S18–S24
- Leduc O, Leduc A. Lymphatic drainage in lymphoedema. Clin Dermatol. 1995;13(5):489–494
- Ezzo J, et al. Manual lymphedema treatment for breast cancer-related lymphedema. Cochrane Database Syst Rev. 2015;(5):CD003475
- NICE. Lymphoedema. London: NICE; 2021. Available at: https://www.nice.org.uk/guidance/conditions-and-diseases/blood-and-immune-system-conditions/lymphoedema
- Dadras M, et al. Post-operative manual lymphatic drainage following liposuction and abdominoplasty: a prospective cohort study. Plast Reconstr Surg. 2017;139(5):1080–1087
- Ekici G, et al. Effectiveness of manual lymphatic drainage therapy in the management of fibromyalgia. J Back Musculoskelet Rehabil. 2009;22(3):163–170
- Schander A, et al. Lymphatic pump treatment increases thoracic duct flow and lymphocyte immune function in normal subjects. Lymphat Res Biol. 2012;10(2):52–58
- Moseley AL, et al. A systematic review of common conservative therapies for arm lymphoedema secondary to breast cancer treatment. Ann Oncol. 2007;18(4):639–646
