
Testosterone Injections for Men — A Complete UK Guide to Injectable TRT
For men with low testosterone, injectable testosterone is one of the most effective and widely used treatment options available in the UK. Depending on the product and dosing schedule, injections may be administered weekly, fortnightly, or as infrequently as every three months — making them a practical choice for men who prefer not to manage a daily routine. This page serves as both a reference guide for men already receiving injectable TRT at The Health Suite and an introduction for men researching their treatment options.
It covers how injectable testosterone works, which products are available in the UK and how they compare, step-by-step intramuscular injection technique, needle selection, sharps disposal, side effects, and what monitoring to expect throughout treatment.
All information should be read alongside the guidance of your prescribing doctor and the Summary of Product Characteristics for your specific medication. It does not constitute medical advice.
What is Injectable Testosterone and How Does it Work?
Injectable testosterone formulations consist of testosterone attached to a fatty acid ester and dissolved in an oil carrier. After intramuscular injection, testosterone is released gradually from the depot formed in the muscle tissue. As it enters the bloodstream, the ester is cleaved away, releasing active testosterone, which then acts on androgen receptors throughout the body to restore normal physiological levels.
The length of the ester chain determines how quickly testosterone is released. Short-chain esters (such as propionate) act quickly but are cleared within days. Longer-chain esters (such as enanthate or undecanoate) release more slowly, sustaining testosterone levels over one to fourteen weeks, depending on the product. This is what makes the wide variation in injection frequency between products possible.
More frequent, smaller doses — for example, twice-weekly rather than fortnightly injections — produce more stable hormone levels day to day, more closely resembling the continuous release profile of testosterone gel. Many specialists favour this approach for this reason.
Injectable Testosterone Products Available in the UK
Four injectable testosterone options are used in the UK for male hypogonadism. Testosterone enanthate and Sustanon 250 are the most commonly used for home self-administration. Nebido is a long-acting depot requiring clinic administration. Testosterone cypionate is not MHRA-licensed in the UK but is prescribed by some private clinics as a licensed import.
| Product | Ester | Oil Carrier | Licensed Interval | Key Points |
| Testosterone Enanthate 250 mg/ml | Enanthate | Castor oil | Every 2–6 weeks (licensed). Weekly or twice-weekly in private practice. | Single-ester preparation — produces predictable, consistent serum levels. Widely available on the NHS. No allergy concern (castor oil carrier). The preferred option for most men self-injecting at home. |
| Sustanon 250 | Four mixed esters (propionate, phenylpropionate, isocaproate, decanoate) | Arachis (peanut) oil | Every 3 weeks (licensed). Weekly in private practice. | CONTRAINDICATED in men with peanut or soya allergy — contains arachis oil. The mixed-ester profile produces rapid early rise followed by slow decline, which can create noticeable symptom fluctuation at the licensed three-weekly interval. Available on the NHS. |
| Nebido 1000 mg/4 ml (testosterone undecanoate) | Undecanoate (longest chain) | Castor oil | Every 10–14 weeks (with 6-week loading injection). | Must be administered by a healthcare professional — not suitable for home self-injection. The 4 ml volume requires a slow, deep intramuscular injection over 2 minutes, with a 30-minute post-injection observation period due to the risk of pulmonary oil microembolism (POME). Available on the NHS. Generic equivalents now licensed in the UK. |
| Testosterone Cypionate 200 mg/ml (unlicensed import) | Cypionate (similar half-life to enanthate) | Cottonseed or olive oil | Weekly or twice-weekly (as prescribed). | Not MHRA-licensed; prescribed under MHRA Regulation 167 as an unlicensed import. Not available on the NHS. Comparable pharmacokinetics to enanthate. Multi-dose vials must be discarded 28 days after first opening. |
Testosterone Enanthate vs Sustanon — Which is Better for Self-Injection?
For the majority of men self-injecting at home, testosterone enanthate has practical advantages over Sustanon. Its single-ester pharmacokinetics produce more consistent and predictable hormone levels. It does not contain arachis oil, so it is safe for men with peanut allergy. Both are available on NHS prescription.
Sustanon’s rapid early rise from the short-chain propionate ester, followed by a slow decline from the decanoate ester, can produce noticeable variation in energy and mood over the injection cycle — particularly when used at the licensed three-weekly interval. Weekly dosing, as used in most private TRT practice, reduces this variation considerably.
How to Self-Inject Testosterone — Step-by-Step
At The Health Suite, testosterone is administered by intramuscular (IM) injection — the licensed route for all UK injectable testosterone products. Your prescribing doctor will specify your product, dose, and injection frequency. Before beginning home self-administration, all patients complete a face-to-face injection training session with a qualified clinic nurse.
First injection training
If this is your first prescription for injectable testosterone at The Health Suite, your nurse will demonstrate and supervise your first injection before you administer at home. Please do not attempt home self-injection without completing this training session first.
Equipment Required
- Drawing-up needle: 18G or 21G — a wider bore draws viscous oil from the ampoule or vial efficiently
- Injecting needle: 21G to 23G (length determined by your body composition — your clinic nurse will advise) — always change to a fresh needle after drawing up
- Luer-lock syringe (1 ml or 2 ml as appropriate) — the locking fitting prevents the needle detaching under oil pressure
- Sterile alcohol swabs
- Sterile cotton ball or gauze
- Approved yellow-lidded sharps bin (BS EN ISO 23907)
- Clean, flat surface — wiped with an alcohol swab before use
Inspect the ampoule or vial before every injection. Do not use if the solution appears cloudy, discoloured, or contains visible particles, and do not use after the expiry date.
How to inject Testosterone
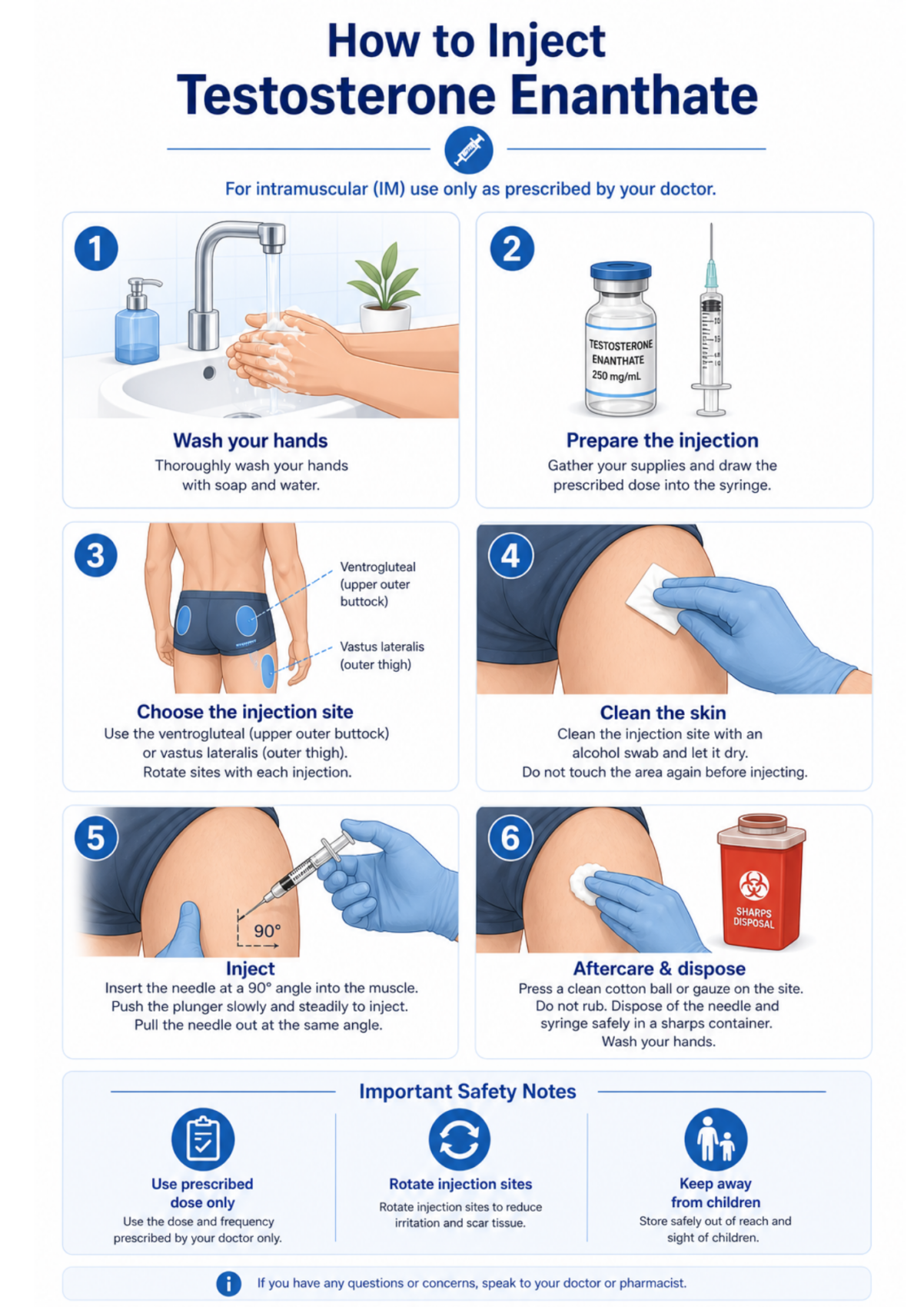
Intramuscular (IM) Injection — Step-by-Step
Intramuscular injection delivers testosterone directly into muscle tissue. It is the licensed route for all UK injectable testosterone products. Nebido (4 ml) must be administered by a healthcare professional and is not suitable for home self-injection.
Needle: 21G to 23G, 25 mm (1 inch) for most men; 38 mm (1.5 inch) for those with greater subcutaneous tissue depth over the injection site. Your clinic nurse will confirm the appropriate length at your training session.
Choosing an Injection Site
- Vastus lateralis (outer thigh) — the recommended site for self-administered IM injection. Use the middle third of the outer aspect of the thigh. A large, accessible muscle with no major neurovascular structures near the surface.
- Ventrogluteal (hip) — considered the safest IM site overall, with the lowest risk of nerve or vessel involvement. Requires correct anatomical landmarking but is achievable with practice. Suitable for self-injection in men with adequate flexibility.
- Dorsogluteal (upper outer buttock) — the traditional site, but increasingly not recommended due to the proximity of the sciatic nerve if positioned incorrectly. It is also difficult to access for self-injection. The ventrogluteal site is the preferred alternative.
- Deltoid (shoulder) — acceptable only for volumes of 1 ml or less. Not a primary site for TRT injections.
- Wash your hands thoroughly with soap and water for at least 20 seconds and dry them on a clean towel.
- Set out equipment on a clean, alcohol-wiped surface. Open the packaging and attach the drawing-up needle to the syringe.
- Clean the ampoule neck or vial bung with an alcohol swab and allow to air dry fully.
- Draw up the prescribed volume. For glass ampoules: snap the neck at the score point (use a snap ring or gauze to protect your fingers), insert the drawing-up needle and withdraw the medication. Draw up marginally more than required, then expel to the correct volume to remove any air.
- Replace the drawing-up needle with the injecting needle. Hold the syringe upright, tap gently to move any bubbles to the top, and advance the plunger slowly until a small drop of oil appears at the tip, confirming the syringe is air-free.
- Clean the chosen IM injection site with an alcohol swab. Allow to dry fully — approximately 30 seconds. Injecting through wet alcohol causes unnecessary stinging.
- Z-track technique: with the non-dominant hand, pull the skin and subcutaneous tissue approximately 1–2 cm sideways, away from the intended needle entry point. Maintain this displacement throughout the injection. When the skin is released after the needle is withdrawn, the displaced tissue seals the needle track, keeping medication within the muscle and reducing injection site reactions.
- While holding the displaced skin, insert the needle firmly and swiftly at 90 degrees to the skin surface.
Inject slowly and steadily over 20 to 30 seconds. Slow injection of oil-based medication is essential — rapid injection is the most common cause of significant injection site pain. - After completing the injection, pause for approximately 10 seconds before withdrawing. This allows pressure to equalise and reduces medication tracking back up the needle path.
- Withdraw the needle at 90 degrees in a single smooth motion. Release the displaced skin — the Z-track seals the deposit within the muscle.
- Apply gentle pressure with sterile gauze. Do not massage the site.
- Dispose of all sharps immediately in the sharps bin.
Tips for Reducing Injection Discomfort
- Bring the medication to room temperature before injecting. Cold oil is more viscous, flows through the needle with greater resistance, and is more uncomfortable. Hold the ampoule or vial in your hands for a few minutes beforehand.
- Ensure the alcohol swab has dried completely before the needle enters the skin.
- Use a fresh needle for every injection. Even a single pass through a rubber vial bung reduces needle sharpness significantly.
- Keep the muscle as relaxed as possible. For thigh injections, sit with the leg hanging freely rather than tense.
- Inject slowly. This is the single most effective measure for reducing pain.
- Rotate injection sites systematically and record which site was used each time.
- A warm compress applied to the site for five to ten minutes after injection encourages oil dispersion and reduces local soreness.
Opening Glass Ampoules
Testosterone enanthate and Sustanon 250 are supplied in glass ampoules. To open safely:
- Tap the top of the ampoule to ensure all medication settles in the lower section.
- Locate the score mark or coloured dot on the neck — this is the intended break point.
- Use an ampoule snap ring or a small square of gauze to protect your fingers.
- Hold the lower section firmly and snap the neck away from you at the score point.
- Dispose of glass ampoule fragments in the sharps bin — not household waste.
Sharps Disposal
Used needles, syringes, and glass ampoule fragments are clinical waste and must be disposed of safely. Incorrect disposal is an offence under the Environmental Protection Act 1990.
- All used sharps must go immediately into an approved sharps container — yellow lid, BS EN ISO 23907 compliant. These are available on NHS FP10 prescription or from The Health Suite.
- Seal the bin when it is three-quarters full. Never overfill.
- Contact your local council for a sharps collection point or door-to-door clinical waste service — most UK councils provide this at no charge.
- Community pharmacies may accept sealed sharps bins for disposal.
- Never place sharps in household bins or recycling.
Dosing, Frequency, Missed Doses, and Travel
Starting Dose and Titration
For testosterone enanthate and cypionate, treatment typically begins at a conservative dose of 62.5 to 125 mg per week, increasing to the minimum dose that achieves symptom relief and a trough serum testosterone in the mid-normal physiological range (generally 15–30 nmol/L). Dose adjustments are made incrementally on the basis of blood results and symptom review, with re-testing four to six weeks after any change. Your prescribing doctor will set and review your dose — do not adjust it independently.
Injection Frequency
More frequent, smaller doses produce more stable hormone levels and reduce the magnitude of post-injection peaks, which lowers the erythropoietic stimulus and risk of haematocrit elevation. For testosterone enanthate and cypionate, twice-weekly injections of half the weekly dose are increasingly preferred over single weekly administration for this reason. Your individual frequency will be agreed at your prescribing consultation and reviewed based on blood results and symptoms.
Missed Dose
If a dose is missed, administer it as soon as it is noticed, provided it is still the same day. If it is the following day and the next scheduled injection is not for several days, administer the missed dose and resume the normal schedule. If the next injection is due shortly, omit the missed dose and continue as planned. Do not double-dose. If uncertain, contact The Health Suite for guidance.
Storage
- Store at room temperature, below 25–30°C depending on the product (confirm in the Summary of Product Characteristics for your specific medication). Protect from direct light.
- Do not refrigerate or freeze injectable testosterone — cold oil becomes unacceptably viscous and the medication may precipitate.
- Multi-dose vials (testosterone cypionate) must be discarded 28 days after first puncture, regardless of remaining volume.
- Inspect for cloudiness, discolouration, or particles before each use. If in doubt, do not use.
- Store out of the reach of children.
Travelling with Injectable Testosterone
Testosterone is classified as a Schedule 4 Part II Controlled Drug under the Misuse of Drugs Regulations 2001. When travelling — particularly abroad — the following precautions are necessary:
- Carry a letter from your prescribing doctor on clinic-headed notepaper, confirming your diagnosis, prescribed medication, dose, and frequency. Include the doctor’s GMC number. The Health Suite can provide this on request.
- Travel with original pharmacy-labelled packaging and a copy of the prescription where possible.
- Carry all injectable medication, needles, and syringes in hand luggage — not checked baggage — to avoid temperature extremes in the hold and the risk of loss.
- Prescription medications are exempt from the 100 ml cabin liquid restriction. A prescriber letter is usually sufficient at UK security.
- For international travel, check the destination country’s regulations on importation of Schedule 4 controlled drugs before departure. Some countries require advance authorisation from their national drugs authority. The Home Office issues a personal export/import licence for up to three months’ supply — contact the clinic if this is required.
Side Effects — What to Expect and What to Report
Injectable testosterone shares the same systemic side effect profile as other forms of TRT, with the addition of injection site-specific effects. The following covers what to expect in practice. Full side effect information is provided in the Summary of Product Characteristics for your product.
Injection Site Reactions
- Pain, redness, swelling, and warmth at the injection site are common, particularly with IM injection and castor oil-based preparations. These typically resolve within 24 to 48 hours. A warm compress, paracetamol or ibuprofen as needed, and consistent site rotation all help.
- Bruising may follow if a small vessel is caught during injection. Apply firm pressure for two to three minutes. Significant or expanding bruising warrants medical review.
Pulmonary Oil Microembolism (POME)
POME is a rare but serious event in which oil enters the venous circulation, typically through inadvertent puncture of a small blood vessel during injection. Symptoms — coughing, breathlessness, chest tightness, dizziness, or faintness — occur within minutes of the injection. The risk is greatest with high-volume IM injections; Nebido (4 ml) carries the highest documented risk, which is why it must be administered clinically with a 30-minute post-injection observation period. If any of these symptoms develop after any injection, sit upright and seek emergency medical attention immediately.
Polycythaemia — The Most Important Safety Consideration
Testosterone stimulates red blood cell production. Injectable testosterone, particularly via the IM route, produces higher and more pronounced post-injection peaks than gel, resulting in a stronger erythropoietic stimulus and a greater tendency for haematocrit to rise. This is the most clinically significant haematological risk of injectable TRT.
- If haematocrit exceeds 54%, the risk of venous and arterial thrombotic events increases. Symptoms of elevated haematocrit include persistent headache, dizziness, visual changes, and a ruddy complexion.
- Per BSSM 2023 guidelines: stop testosterone if haematocrit exceeds 54%; do not restart until it falls below 50%; investigate for secondary causes.
- Management options: dose reduction, switch to a lower-peak formulation (such as gel), or therapeutic phlebotomy.
- Risk factors for polycythaemia on TRT: smoking, obstructive sleep apnoea, obesity, older age, and higher testosterone peaks from infrequent IM dosing.
Other Systemic Side Effects
- Acne and oily skin — more pronounced at higher doses or when significant post-injection peaks occur.
- Fluid retention and weight gain — usually mild; monitor blood pressure.
- Worsening obstructive sleep apnoea — inform your prescribing doctor of any new or worsening snoring, choking episodes during sleep, or significant daytime somnolence.
- Gynaecomastia — breast tissue development due to aromatisation of testosterone to oestradiol, more pronounced at higher levels.
- Mood changes — irritability and mood fluctuation are most prominent when pronounced peaks and troughs occur with infrequent dosing. More frequent, lower-dose injections typically reduce this.
- Elevated PSA — expected at physiological testosterone levels and monitored routinely. There is no current evidence that testosterone causes de-novo prostate cancer. The TRAVERSE trial (Lincoff et al., NEJM, 2023) found no significant increase in prostate cancer incidence in 5,204 hypogonadal men treated with testosterone gel versus placebo over 33 months.
When to Seek Emergency Care
- Sudden leg pain, swelling, or redness — possible deep vein thrombosis. Call 999.
- Sudden breathlessness, chest pain, or coughing blood — possible pulmonary embolism or POME. Call 999.
- Persistent erection lasting more than four hours (priapism) — attend A&E immediately.
- Symptoms of POME within minutes of injection (coughing, breathlessness, dizziness) — call 999.
Contraindications
Injectable testosterone must not be used in men with known or suspected prostate cancer, breast cancer, or documented hypersensitivity to testosterone or the oil carrier. Sustanon is specifically contraindicated in men with a peanut or soya allergy. Use with caution in men with obstructive sleep apnoea, thrombophilia, epilepsy, or pre-existing polycythaemia. All contraindications are assessed at the initial clinical consultation before any prescription is issued.
Monitoring Appointments — What to Expect
Ongoing monitoring is an essential part of safe injectable TRT, not an optional add-on. It ensures that testosterone levels remain in the optimal range, that your red blood cell count is within safe limits, and that the treatment continues to work well for you. At The Health Suite, blood tests are scheduled at 3, 6, 9, and 12 months in the first year, then annually once levels are stable.
Before Treatment Begins
Baseline blood tests are completed before your first prescription. These establish a clinical starting point covering testosterone levels (two fasting morning samples), red blood cell count, PSA if you are over 40, liver function, cholesterol, blood sugar, and a full symptom assessment. Treatment is initiated only once this picture is complete.
3 Months
The first follow-up checks that your testosterone level has reached the target range and that haematocrit — the most time-sensitive safety marker with IM injectable TRT — is within acceptable limits. Your prescribing doctor will also review symptoms including energy, mood, libido, and any side effects. If a dose or frequency adjustment is needed, it is made here and re-tested at the next scheduled appointment.
6 Months
A mid-year review covering testosterone levels, haematocrit, PSA if applicable, and ongoing symptom assessment. This appointment confirms the treatment is continuing to work well and allows any further refinements to dose or frequency before the nine-month check.
9 Months
A further blood test and clinical review. By this point most patients are on a stable, optimised dose. This appointment provides an opportunity to catch any emerging changes in haematocrit or PSA before the full twelve-month review, and to assess ongoing symptom response.
12 Months — Full Annual Review
A comprehensive review at the end of the first treatment year covers testosterone levels, haematocrit, PSA, liver function, lipid profile, blood pressure, and BMI, alongside a full symptom assessment. After this point, provided levels are stable and there are no safety concerns, monitoring moves to an annual cycle.
Annually Thereafter
Annual reviews continue indefinitely for as long as treatment is maintained, covering the same full panel as the twelve-month review. If anything changes between scheduled appointments — symptoms shift, a new side effect develops, or a health concern arises — contact The Health Suite to arrange an earlier assessment rather than waiting for the next scheduled review.
Frequently Asked Questions
Starting Injectable TRT at The Health Suite
The Health Suite provides comprehensive testosterone replacement therapy at our CQC-registered private clinic in Thurnby, Leicester — from initial consultation and laboratory assessment through to prescription, injection training, and full ongoing monitoring. Treatment is prescribed by experienced doctors working within current UK clinical guidelines.
Assessment begins with a clinical consultation and baseline blood tests. For men already on testosterone treatment elsewhere and considering transferring their care, our doctors can review existing results and discuss the most appropriate pathway.
Book a TRT consultation at The Health Suite
Appointments available in Leicester for new and existing patients. Our doctors specialise in men’s hormone health and take an integrative approach to testosterone deficiency, addressing the full clinical picture rather than the number alone.
Testosterone Replacement Therapy
Expert-Led Testosterone Replacement Therapy in The Health Suite Leicester
References and Clinical Guidelines
Have a query about Testosterone Injections for Men — A Complete UK Guide to Injectable TRT?
We recognise that getting the healthcare assistance you need can be difficult. So if you have a query, feel free to contact us and one of our treatment co-ordinators will be happy to help. We aim to reply to all queries within 24 hours (Mon – Fri).
