Functional Medicine for ADHD: Can Nutrition and Gut Health Help?
Attention Deficit Hyperactivity Disorder (ADHD) is one of the most commonly diagnosed neurodevelopmental conditions in both children and adults, yet the conversation around its management has for decades been dominated almost entirely by medication. Stimulant medications remain the most extensively researched and widely used interventions, and for many people they produce significant and meaningful improvements in attention, impulse control and daily functioning.¹ But medication does not work for everyone, and even for those it does help, it rarely addresses the full picture.
A growing body of research has begun to explore the relationship between nutritional status, gut health, inflammation and ADHD symptom severity.
And this research is raising legitimate questions about whether what we eat, and the state of our digestive system, might be meaningfully influencing the neurobiology that underlies the condition.² Understanding what the evidence actually shows, and where the genuine uncertainties remain, is important for anyone considering a broader approach to managing ADHD.
What Is Functional Medicine
Functional medicine is an approach to healthcare that seeks to identify and address the underlying biological, environmental and lifestyle factors contributing to a condition, rather than focusing solely on symptom suppression.
It draws on conventional medical science while integrating nutritional biochemistry, gut physiology, environmental medicine and lifestyle factors into a coherent clinical picture for each patient.³
In the context of ADHD, a functional medicine approach does not replace established diagnosis and treatment. Rather, it asks a different set of questions alongside them, such as:
- Are there nutritional deficiencies that may be impairing the synthesis or regulation of neurotransmitters relevant to attention and executive function?
- Is there evidence of gut dysbiosis or intestinal permeability that might be driving systemic inflammation?
- Are dietary patterns contributing to blood sugar instability that worsens focus and behavioural regulation?
- Could food sensitivities be provoking an immune response that affects brain function?
These are not fringe questions. They are increasingly the subject of peer-reviewed research, with results that are substantive enough to warrant serious clinical consideration and application.
For adults who have received a diagnosis and are exploring their management options, or for those who suspect their difficulties with concentration, organisation and impulse control may have a nutritional or physiological dimension, a functional medicine assessment offers a structured and evidence-grounded route to answers.
The Gut-Brain Axis and ADHD
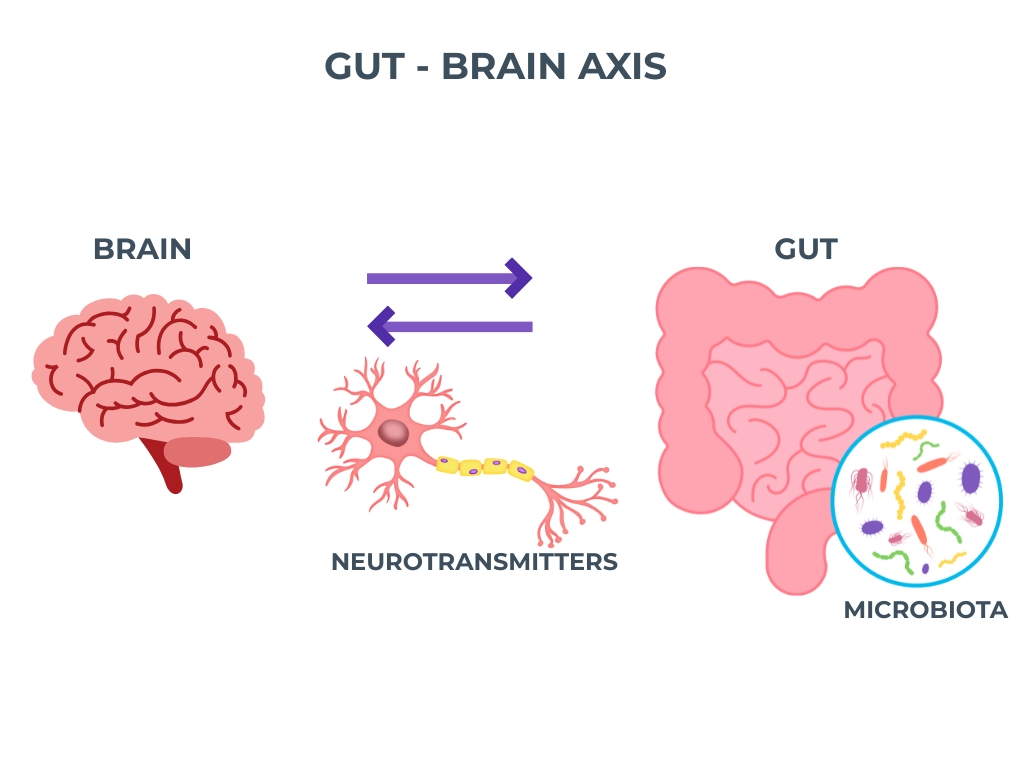
The gut-brain axis, the bidirectional communication network between the enteric nervous system of the gastrointestinal tract and the central nervous system, has emerged as one of the most significant areas of neuroscience research over the past decade.
The gut microbiome, comprising the trillions of bacteria, fungi and other microorganisms that inhabit the digestive tract, plays a central role in this communication, influencing the production of neurotransmitters, the regulation of the immune system and the modulation of inflammatory pathways that extend to the brain.
A landmark review published in Physiological Reviews described the microbiota-gut-brain axis as a complex, bidirectional signalling system with far-reaching implications for neurological and psychiatric health.⁴
Approximately 90% of the body’s serotonin is produced in the gut, and the microbiome also influences the production of dopamine precursors, short-chain fatty acids and other metabolites that have direct effects on brain function and behaviour.⁵
Given that ADHD is characterised in part by dysregulation of dopaminergic and noradrenergic signalling, that biological link between ADHD symptom severity and gut comes into focus in meaningful ways.
Research investigating this relationship has found meaningful differences in gut microbiome composition between individuals with ADHD and neurotypical controls, with studies identifying reduced microbial diversity and alterations in the relative abundance of specific bacterial genera.
That direction of causality, whether gut dysbiosis contributes to ADHD or ADHD-related behaviours and dietary patterns contribute to dysbiosis, remains an active area of investigation.⁶
What is clear is that the gut-brain axis represents a plausible and increasingly evidenced pathway through which ADHD gut health interventions might influence neurobiology, and that the relationship between the two deserves serious clinical attention.
Chronic low-grade inflammation adds another layer to this picture. Increased intestinal permeability, sometimes referred to informally as leaky gut, describes a state in which the integrity of the intestinal barrier is compromised, allowing bacterial products to enter circulation and trigger immune activation.⁷
There is growing evidence that neuroinflammation, driven partly by systemic inflammatory signals originating in the gut, may play a role in the pathophysiology of several neurodevelopmental and neuropsychiatric conditions including ADHD.⁸
Dietary interventions that support gut barrier integrity, including adequate fibre, fermented foods and reduction of ultra-processed food consumption, may therefore have indirect benefits for neurological function alongside their broader health value.

Nutritional Deficiencies and ADHD Symptom Severity
Several specific nutritional deficiencies have been associated with ADHD symptom severity, and addressing them through diet or supplementation represents one of the most evidence-supported components of a functional medicine approach. The deficiencies most consistently implicated in the research literature are iron, zinc, magnesium, omega-3 fatty acids and vitamin D, and each operates through mechanisms that are biologically relevant to the neurotransmitter systems and brain regions involved in ADHD.
Iron is essential for the synthesis of dopamine, and low iron status, even at levels that do not produce clinical anaemia, has been consistently associated with more severe ADHD symptoms. Studies have found that serum ferritin levels are significantly lower on average in people with ADHD than in controls, and that supplementation in iron-deficient individuals can produce improvements in attention and behavioural regulation.⁹
Zinc plays an important role in the metabolism of dopamine and in the regulation of melatonin, which in turn influences dopamine levels in the prefrontal cortex, and lower zinc levels have been found across multiple studies of people with ADHD.¹⁰ Magnesium is involved in over 300 enzymatic reactions, including those relevant to neurotransmitter synthesis, and deficiency has been reported at elevated rates in children and adults with ADHD, alongside associations with hyperactivity, inattention and emotional dysregulation.¹¹
The evidence for omega-3 fatty acids is among the most robust of any nutritional intervention in ADHD. EPA and DHA, the long-chain omega-3 fatty acids found in oily fish and fish oil supplements, are essential structural components of neuronal cell membranes and play a key role in dopaminergic and serotonergic neurotransmission. A meta-analysis published in Neuropsychopharmacology found that omega-3 supplementation produces small but statistically significant improvements in attention, hyperactivity and impulsivity, with an effect size comparable to some non-stimulant medications.¹²
Vitamin D receptors are found throughout the brain, including in the prefrontal cortex and limbic system, and low vitamin D levels have been associated with increased ADHD symptom severity in multiple studies, making this a particularly relevant consideration in the UK population, where deficiency is extremely prevalent.¹³ Assessing nutritional status through targeted laboratory testing is therefore a clinically meaningful step in any comprehensive ADHD evaluation, given that deficiencies in these micronutrients are common, may go undetected without specific testing, and are addressable through straightforward dietary or supplementation interventions.
Dietary Patterns, Blood Sugar Regulation and ADHD Nutrition
Beyond specific micronutrients, broader dietary patterns appear to influence ADHD symptom severity through several mechanisms, and ADHD nutrition is increasingly recognised as a legitimate clinical consideration rather than an alternative medicine preoccupation. Diets high in ultra-processed foods, refined carbohydrates and added sugars are associated with greater symptom burden in both children and adults with ADHD, while diets characterised by higher intake of vegetables, whole grains, lean proteins and healthy fats are associated with lower symptom severity.¹⁴
Blood sugar regulation is a particularly important mechanism here. The prefrontal cortex, the brain region most implicated in the executive function deficits that define ADHD, is highly sensitive to fluctuations in glucose availability. Rapid rises and falls in blood sugar, produced by high-glycaemic diets and irregular eating patterns, can transiently impair prefrontal function and worsen attention, impulse control and emotional regulation.
A review published in Nature Reviews Neuroscience highlighted the extent to which dietary composition directly influences neurotransmitter availability and cognitive function across multiple domains.¹⁵ Stabilising blood sugar through a diet that emphasises low-glycaemic foods, adequate protein and regular meals is therefore a practical and evidence-based dietary strategy for people managing ADHD.
Additionally, a landmark trial published in The Lancet found that 64% of participants showed a clinically meaningful reduction in ADHD symptoms on a restricted elimination diet, suggesting that food sensitivities represent a genuine aetiological contributor in a significant minority of cases.16 This does not mean dietary elimination is appropriate for everyone, but in individuals whose symptoms fluctuate in relation to dietary intake, or who present with co-existing signs of food sensitivity, a structured assessment of dietary triggers under specialist guidance is clinically warranted.
A Functional Medicine Approach in ADHD
A functional medicine assessment for an individual with ADHD begins not with a treatment protocol but with a thorough investigation of the individual’s biochemical, nutritional and lifestyle context. This typically involves a detailed dietary history, targeted laboratory testing to identify relevant deficiencies and markers of inflammation or gut dysfunction, and a clinical assessment of factors including sleep quality, stress, exercise patterns and co-existing health conditions that may be influencing symptom severity.17
The resulting plan is genuinely personalised. It might include targeted nutritional supplementation to address identified deficiencies, dietary modifications to improve blood sugar stability and reduce inflammatory load, probiotic or prebiotic interventions to support microbiome diversity, and lifestyle recommendations around sleep and physical activity. For many adults, this approach sits alongside medication and other therapeutic interventions, addressing biological variables that conventional ADHD management does not routinely assess.
The goal is not to replace established treatment but to ensure that the full range of factors shaping a person’s experience of ADHD is identified and, where possible, addressed. This matters because ADHD in adulthood is not simply a concentration problem. It shapes how people organise their time, manage their relationships, sustain their motivation and regulate their emotions across every domain of daily life.
An approach that engages seriously with the nutritional and physiological context of those difficulties, rather than treating medication as the only available lever, is one that respects the complexity of the condition and the individuality of the person living with it.
Adult ADHD Assessment at The Health Suite Leicester
If you are struggling with focus, organisation, impulsivity or the chronic sense of being behind that many adults with ADHD describe, a comprehensive assessment is the essential first step toward clarity and effective management.
At The Health Suite Leicester, our adult private ADHD diagnostic assessments are conducted by consultant psychiatrists and provide a thorough evaluation of your symptoms, personal history and daily functioning. However, we go beyond just a diagnosis; our functional medicine doctors will review you more holistically. By going beyond the diagnosis to explore the full scope of your experience, developing a tailored action plan that may include recommendations for further functional medicine testing, therapy, supplements, lifestyle adjustments or nutritional support, designed to help you lead a more focused, organised and fulfilling life.
We understand that many adults reach us having spent years attributing their difficulties to other causes. Our goal is to offer not only clinical accuracy but genuine understanding, providing the clarity and compassionate support needed to make meaningful and lasting change.
Functional Medicine ADHD Support for Adults, Children & Teenagers services
Find out more about our Functional Medicine ADHD Support for Adults, Children & Teenagers services at The Health Suite Leicester and book a consultation today:
Functional Medicine ADHD Support for Adults, Children & Teenagers
A Specialist-Led, Integrative Approach to ADHD in Leicester - Helping you or your child improve focus, energy, emotional balance and wellbeing
Related Services
Child ADHD Assessment
Consultant-Led Child ADHD Assessment Services at The Health Suite Leicester
Adult ADHD Assessment
Private Adult Private ADHD Assessments with Consultant Psychiatrists at The Health Suite Leicester
ADHD Medication Prescribing
Expert Private ADHD Medication Prescribing in Leicester
References
Have a query about Functional Medicine for ADHD: Can Nutrition and Gut Health Help??
We recognise that getting the healthcare assistance you need can be difficult. So if you have a query, feel free to contact us and one of our treatment co-ordinators will be happy to help. We aim to reply to all queries within 24 hours (Mon – Fri).