Top Daily Habits That Could Be Making Your TMJ Pain Worse (And How to Fix Them)
Temporomandibular joint disorder, more commonly known as TMJ, is one of those conditions that has a habit of becoming a constant, low-level presence in daily life before a person fully recognises what is driving it.
The jaw aches in the morning. There is a clicking sound when eating. Headaches arrive without an obvious cause. The neck and shoulders feel permanently tense. The ears feel blocked or uncomfortable for no apparent reason. Individually, each of these things seems manageable. Together, they can significantly affect concentration, sleep, eating and general quality of life.
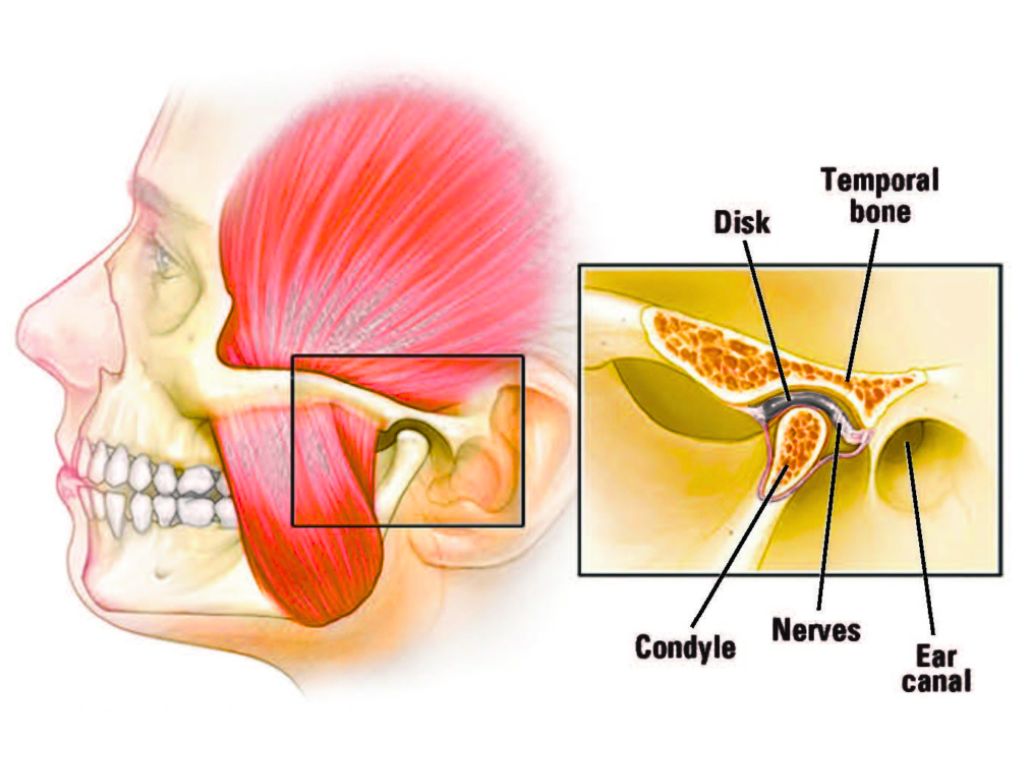
What makes TMJ disorder particularly frustrating is that many of the habits and behaviours that sustain it are things people do without thinking, patterns so deeply embedded in daily routine that they feel entirely normal. This is all the more important when you consider that the temporomandibular joint is one of the most complex joints in the body, combining hinge and sliding movements to allow the jaw to open, close, move sideways and protrude [1].
It sits directly in front of the ear on each side of the face, which is why TMJ disorder so frequently produces symptoms that extend well beyond the jaw itself, including earache, a sensation of fullness or ringing in the ears, temple headaches, facial pain and neck and shoulder tension [2].
Know more abot TMJ
Many people spend months attributing these symptoms to ear infections, migraines or cervical spine problems before the jaw is identified as the source.
The joint is also one of the most heavily used in the body, involved in speaking, eating, swallowing and breathing, functions that occur hundreds of times each day. When the joint, its surrounding muscles or the disc that cushions it becomes inflamed, overloaded or displaced, the resulting pain and dysfunction can be both wide-ranging and persistent [2][3]
TMJ affects an estimated 5–12% of the population, with higher prevalence in women and in adults between the ages of 20 and 40 [3].
Yet despite its prevalence, it remains significantly underdiagnosed, with many people managing symptoms for years without understanding their cause or knowing that effective treatment is available.

Understanding which daily habits are contributing to the problem, and what to do about them, is often the most important step in breaking the cycle.
1. Clenching and Grinding
Bruxism, the habitual clenching or grinding of the teeth, is one of the most significant contributors to TMJ pain and one of the most common [4]. It can occur during the day, often triggered by concentration, stress or anxiety, or during sleep, where the person has no conscious awareness of it at all. Sleep bruxism in particular places an enormous load on the temporomandibular joint and the muscles of mastication, with research suggesting that the forces generated during sleep grinding can be several times greater than those produced during normal chewing [5]. The challenge with daytime clenching is that most people do not notice they are doing it. The jaw quietly tightens during a difficult phone call, a demanding piece of work or a stressful commute, and by the time the person becomes aware of the tension, the muscles have already been under sustained load for an extended period.
Making a conscious habit of checking jaw position throughout the day is one of the most effective behavioural interventions available. The teeth should not be touching when the mouth is at rest. The lips should be lightly closed, the teeth slightly apart, and the tongue resting gently on the roof of the mouth [6]. Setting a periodic reminder to check and release jaw tension, particularly during activities known to trigger clenching, can produce meaningful reductions in muscle load over time.
For sleep bruxism, an occlusal splint or night guard, custom-fitted by a dental professional, remains the most commonly recommended intervention for protecting the joint and the teeth from the effects of nocturnal grinding [7].
While a splint does not eliminate bruxism, it distributes the forces more evenly and reduces the compressive load on the joint during sleep.
2. Chewing Habits
The jaw muscles are among the strongest in the body relative to their size, but they are not designed for sustained, repetitive loading beyond what normal eating requires.8 Habits that impose additional or asymmetrical load on the joint can drive inflammation and muscle fatigue in ways that significantly worsen TMJ symptoms. Chewing gum is one of the most common offenders. What feels like a relatively minor activity involves sustained bilateral contraction of the masseter and temporalis muscles, and for someone with an already irritated temporomandibular joint, even a short period of gum chewing can trigger or significantly worsen pain [9].
Eliminating chewing gum entirely is one of the simplest and most immediate changes a person with TMJ disorder can make. Chewing predominantly on one side of the mouth, often a habit developed unconsciously to avoid a painful tooth or a poor bite, places an asymmetrical load on the joint and can drive muscular imbalance and joint inflammation on the overloaded side [10].
Making a conscious effort to distribute chewing more evenly and choosing softer foods during periods of acute pain reduces the mechanical load on the joint and gives the surrounding tissues an opportunity to recover. Hard, chewy or crunchy foods, including raw carrots, hard bread crusts, tough meat and ice, require the jaw to generate high closing forces and can provoke significant pain in an already sensitised joint [6][9].
During symptomatic periods in particular, a temporarily modified diet that avoids these foods can make a meaningful difference to daily pain levels.
3. Posture and Jaw Position
The relationship between posture and TMJ pain is well established and frequently underappreciated. The head, neck and jaw function as an integrated mechanical system, and changes in the position of one component inevitably affect the others [11]. Forward head posture, a pattern in which the head sits forward of the shoulders rather than directly above them, is among the most common postural problems in modern life, driven by prolonged screen use, desk work and smartphone habits.
Research published in the Journal of Oral Rehabilitation found a significant association between forward head posture and the presence and severity of TMJ disorder symptoms, with the altered cervical alignment placing increased load on the muscles of mastication and the temporomandibular joint itself [12]. Correcting forward head posture requires attention to workstation ergonomics, screen height and sitting position, as well as targeted physiotherapy or exercise to strengthen the deep cervical flexors and restore normal cervical alignment [11][12].
These changes do not produce immediate results, but sustained improvement in posture can produce meaningful reductions in TMJ-related muscle tension over time. Resting the chin or jaw on the hand, a habit many people adopt unconsciously while reading, thinking or working at a desk, applies direct lateral force to the mandible and can displace or compress the joint in ways that worsen pain [6].
Becoming aware of this habit and breaking it is a small change that can have a disproportionate impact on symptom levels.
4. Stress and Emotional Tension
The connection between psychological stress and TMJ disorder is one of the most robustly evidenced relationships in the field. A systematic review published in the Journal of Dental Research found that psychological stress was significantly associated with both the onset and severity of TMD symptoms, with the relationship mediated in part through increased muscle tension, bruxism and altered pain sensitivity [13].
Stress not only drives clenching and grinding. It also lowers the threshold at which pain is perceived, meaning that the same level of joint loading that would be tolerable in a calm state can produce significant pain when a person is anxious, sleep-deprived or under sustained pressure [14]. This is why TMJ symptoms so often worsen during periods of life stress and improve when circumstances ease, even without any direct intervention on the joint itself. Developing effective stress management strategies is therefore not peripheral to TMJ management but central to it.
Evidence-based approaches, including cognitive behavioural therapy, mindfulness-based stress reduction and progressive muscle relaxation, have all demonstrated benefit in reducing TMD symptom severity, with the greatest effects seen in patients whose symptoms have a significant stress-related component [15].
Regular physical activity, adequate sleep and attention to work-life balance contribute to the same outcome by reducing the background level of physiological arousal that drives muscle tension.
5. Sleep Position
Sleep position is another area where small changes can produce meaningful improvements in TMJ symptoms, yet it is one of the last things most people consider when managing jaw pain. Sleeping on the stomach requires the head to be rotated to one side for an extended period, placing sustained asymmetrical load on the cervical spine and the temporomandibular joint and driving the muscular imbalances that contribute to pain. Side sleeping, particularly on the same side every night, can also place direct pressure on the jaw and compress the joint. Back sleeping, with a supportive pillow that maintains neutral cervical alignment, is the position most likely to reduce loading on the temporomandibular joint during sleep [6][16].
For people who find it difficult to change sleep position, a body pillow that prevents rolling onto the stomach or the habitual side can help to maintain a more neutral sleeping posture through the night.
6. Oral Habits
A range of oral habits beyond bruxism can contribute to TMJ pain by placing repeated or sustained load on the joint and its surrounding structures. Nail biting, pen chewing, biting the inside of the cheek and chewing on hard objects all involve the kind of repetitive, often asymmetrical jaw loading that irritates an already sensitised joint [9].
These habits are frequently driven by anxiety or concentration and may be so automatic that the person is barely aware of them. Identifying and interrupting these patterns, using strategies such as keeping the hands occupied, using a stress ball or applying a bitter-tasting nail deterrent, can reduce their frequency significantly. Opening the mouth very wide, whether yawning, eating a large sandwich or during dental treatment, can strain the joint capsule and the surrounding ligaments and is a common trigger for acute pain flares in people with TMJ disorder [6].
Being conscious of avoiding extreme mouth opening during symptomatic periods and supporting the jaw gently when yawning can prevent unnecessary provocation of the joint.
When to Seek Specialist Assessment
Self-management of daily habits is an important part of TMJ disorder management, but it works best when it is informed by an accurate diagnosis and guided by specialist clinical input. Many people spend months or years modifying their behaviour based on an incomplete understanding of what is driving their symptoms, when a thorough assessment would reveal the specific mechanical, muscular or joint-related factors at play and allow a more targeted treatment approach.
In fact, a systematic review published in the Journal of Orofacial Pain found that patients who received specialist assessment and a structured, multimodal treatment plan, combining behavioural advice, physiotherapy, occlusal management and, where indicated, psychological support, achieved significantly better long-term outcomes than those managed with self-directed behaviour change alone [17].
A specialist assessment for TMJ disorder typically includes a detailed history of symptoms and their triggers, clinical examination of the joint and the muscles of mastication, assessment of bite and occlusion, and, where indicated, imaging to evaluate the joint structures and disc position [18]. From this, a personalised treatment plan can be developed that addresses the specific drivers of the individual’s symptoms rather than applying a generic approach.
TMJ Assessment and Treatment at The Health Suite Leicester
If jaw pain, headaches, clicking, ear discomfort or facial tension have become a feature of daily life, and self-management alone has not provided the relief you were hoping for, a specialist assessment can identify exactly what is driving your symptoms and what treatment is most likely to help.
At The Health Suite Leicester, our TMJ assessments are thorough and consultant-led. We take a detailed history, examine the joint and surrounding musculature, assess bite and jaw mechanics, and develop a personalised treatment plan that may include: Osteopathy, Craniosacral Therapy and Buccal Facial Massage.
TMJ disorder is a genuinely treatable condition, and most people see meaningful improvement with the right combination of clinical support and targeted habit change. You do not have to manage it alone.
Find out how specialist TMJ assessment and treatment at The Health Suite Leicester can help you move forward by booking your appointment today:
TMJ Treatment
Multidisciplinary TMJ care at The Health Suite Leicester | Jaw Pain, Clicking & Tension Support
References
Have a query about Top Daily Habits That Could Be Making Your TMJ Pain Worse (And How to Fix Them)?
We recognise that getting the healthcare assistance you need can be difficult. So if you have a query, feel free to contact us and one of our treatment co-ordinators will be happy to help. We aim to reply to all queries within 24 hours (Mon – Fri).